Share:
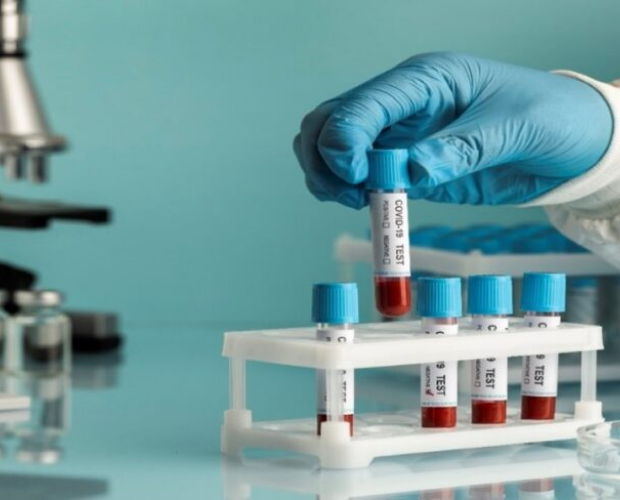
In May 2022, Arshita Mahesh Aggarwal, the daughter of a high-ranking IPS officer, experienced a distressing situation during a home blood test in Chennai. After paying Rs.950 for the service, the phlebotomist’s* negligence left her with a painful bruise and a questionable report. The lab indicated her T4 (thyroxine) level was 5.6 nmol/L, starkly outside the reference range of 52 to 127 nmol/L. This alarming result led to considerable stress and a whirlwind of medical consultations, only for a retest at another lab to reveal normal levels. Seeking justice, Arshita approached the Chennai District Consumer Disputes Redressal Commission for compensation.
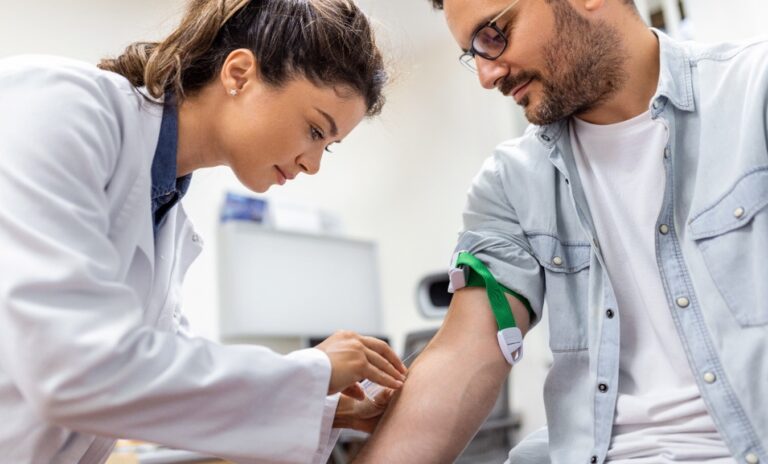
*Phlebotomy – the drawing of blood – has been practised for centuries and is still one of the most common invasive procedures in health care. Each step in the process of phlebotomy affects the quality of the specimen and is thus important for preventing laboratory error, patient injury and even death. For example, the touch of a finger to verify the location of a vein before insertion of the needle increases the chance that a specimen will be contaminated.
The lab dismissed the error as typographical, but the real issue might lie in the pre-analytic phase of sample collection. This phase, encompassing the time from sample collection to lab processing, is critical and particularly challenging in home sample collection. Temperature control plays a pivotal role, as samples must be maintained between 2-8°C to remain viable.
 Designed by Freepik
Designed by Freepik
In India’s scorching climate, this requirement is difficult to meet, especially when samples are transported over long distances.
Blood samples exposed to extreme temperatures can undergo biochemical changes that compromise their integrity.
Blood is a complex mixture of cells, proteins, enzymes, and molecules. Temperature fluctuations can cause proteins to denature, enzymes to deactivate, and cells to degrade. These changes lead to inaccurate test results and potential misdiagnoses, jeopardizing patient care.
According to the University of California, Los Angeles, blood components should be stored as follows:
Red blood cells can be stored for up to 42 days at 1°C to 6°C, depending on additive.
Platelets can be stored at 20°C to 24°C for up to 5 days with constant agitation.
Plasma that is frozen at temperatures of -18°C or below within 8 hours of collection, platelets can be stored for up to 1 year.
Designed by Freepik
To combat these challenges, thermal energy storage materials like Phase Change materials (PCM) are yet not fully exploited to its potential. The combination of PCM, insulation and its selection offers the thermal packaging industry to innovate and engineer thermal packaging solutions that solve several problems around precise and safe transport of diagnostic samples.
These materials offer an array of temperature options to create a robust, foolproof and custom solution depending on the required temperature, duration and criticality. PCMs are at the forefront of this innovation. PCMs absorb or release energy as they change phase, providing precise temperature control. Unlike traditional ice, PCMs offer long-lasting thermal stability.

Courtesy: RGEES LLC/Paradigm – Innovative sample carrier which doubles up as the PCM coolant carrier offering a robust protection
When designed with a phase transition temperature matching the ideal storage range, PCMs ensure samples remain within the 2-8°C window, even in extreme conditions.
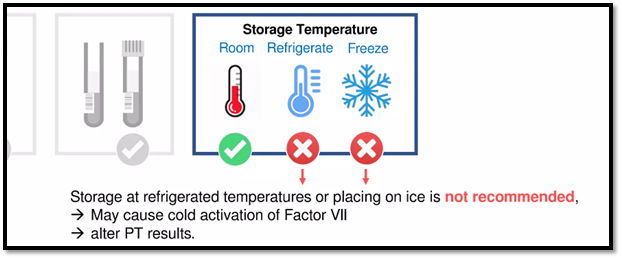
Pre-validated temperature-controlled packaging using PCMs can maintain the critical 2-8°C range. This technology not only prevents temperatures from rising above 8°C but also keeps them from dropping below 2°C, even during India’s hot summers.
For certain samples such as for blood platelets which require controlled room temperature which is defined as +15 to +25°C. Selection of specific PCM designed to maintain this range is used instead of using gel packs or ice packs which are not recommended.
Whole blood intended for platelet separation must be maintained at +20 to +24°C prior to processing, as lower temperatures can impair platelet function and their separation efficiency. Platelets should be prepared within 8 hours of blood collection and stored at 20-24°C with continuous agitation to prevent aggregation, which could compromise their viability. Depending on the type of blood bag used, platelets have a shelf life of 3-5 days. Due to the room temperature storage, there is a risk of bacterial contamination; hence, the storage area should consistently remain below 24°C. During transport, platelets should be kept in a blood transport box that maintains a temperature range of 20-24°C. Platelets must not be refrigerated and should be transfused as soon as possible.
Implementing PCM-based temperature-controlled packaging in sample transportation could transform healthcare diagnostics. Reliable temperature control ensures accurate test results, reducing stress for patients and their families.
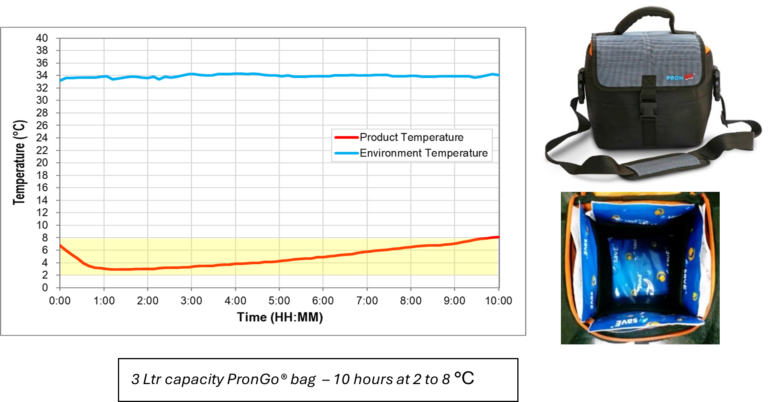
PCM based range of products like the Prongo® bag and Celsure® from Pluss demonstrates the efficacy of PCM-based solutions in real-world condition;
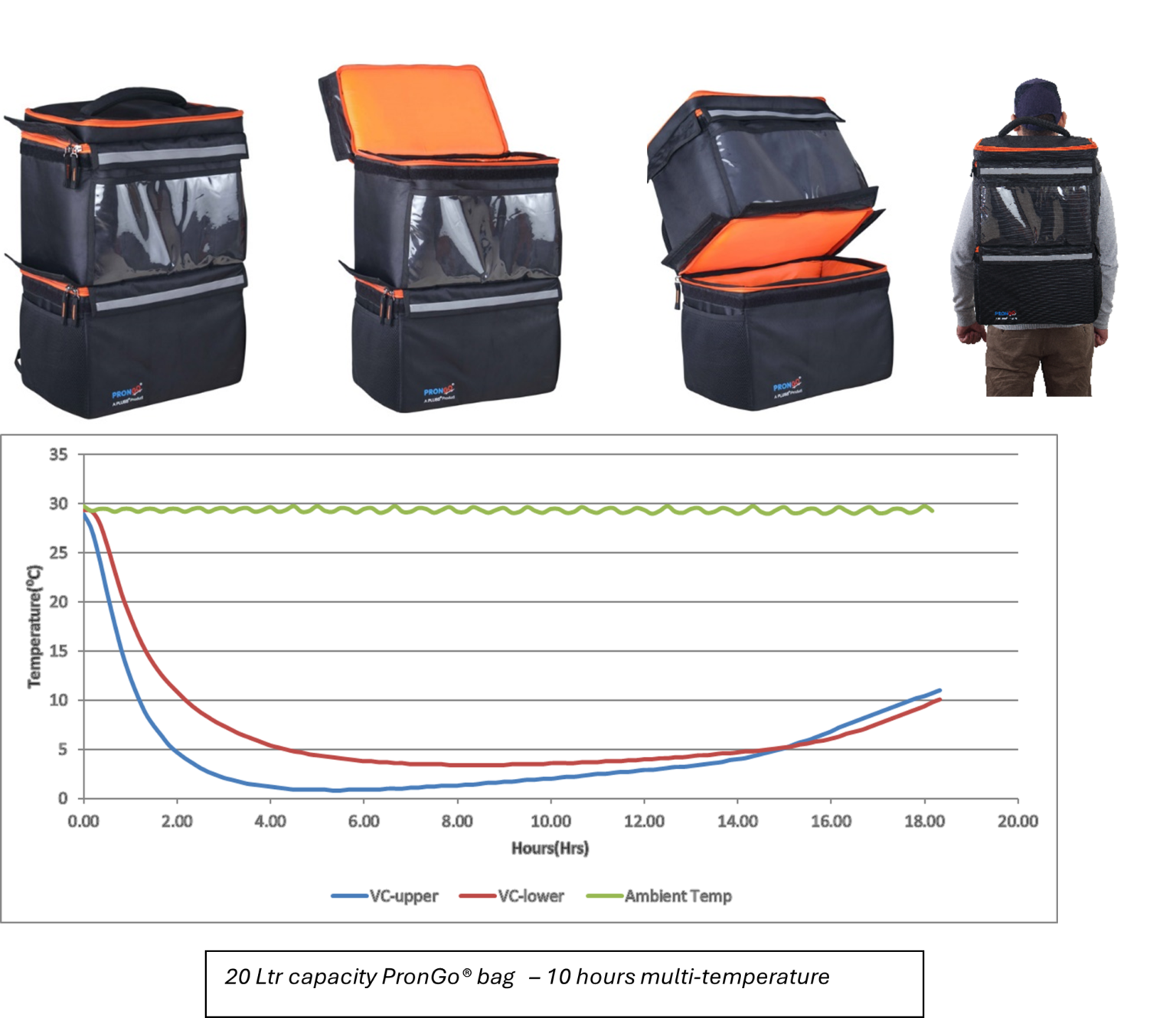
More examples of different form factors and design to enable operational ease and functional enhancements shown in the images below;

Arshita’s story highlights the critical importance of proper sample transportation in healthcare diagnostics. Embracing innovative solutions like thermal energy storage with PCMs can mitigate temperature-related risks and ensure the reliability of test results. It’s time to execute on and embrace technologies in materials, thermal engineering and digital integration which are today available towards development of future of blood sample collection & transportation in healthcare.
Author: Deepika Singhal & Vishnu Sasidharan
Contributor: Raman Chauhan
© 2024. All Rights Reserved.
We use cookies to personalise content and ads, to provide social media features and to analyse our traffic. We also share information about your use of our site with our social media, advertising and analytics partners who may combine it with other information that you’ve provided to them or that they’ve collected from your use of their services.

Udit is a management post-graduate specializing in Marketing & Finance from Management Development Institute (MDI) Gurgaon and has a Bachelors in Technology in Biotechnology from Amity University, Noida, India. Udit has over 11 years of experience in the area of life sciences and healthcare. Before joining at PLUSS, he has held different roles ranging from product management to business management in companies from life science industry such as Bio-Rad Laboratories and Thermo Fisher Scientific. Udit now leads healthcare and agriculture business verticals at PLUSS - from strategizing the new product development to identifying business growth opportunities. He has been a recipient of several awards in his previous roles and has also been a speaker at different public and private conferences. One of the latest innovations he is working on is an affordable, electricity free infant warmer for low birth weight new born babies supported by BIRAC and CMC Vellore.
Besides work, Udit has keen interest in a variety of subjects that he enjoys fueling through reading and traveling. His interests range from colonial history to advances achieved in science and technology; from philosophy to finance and; from chess to cricket.
Preeti is a seasoned professional with an impressive academic background in engineering, HR management, and law. Her career journey began with Siemens India, where she excelled in both Technical and HR functions. She later transitioned to Executive Search and Recruiting, where she thrived as both a Consultant and Entrepreneur.
Preeti's expertise is deeply rooted in a people-centric approach, which she brought to PLUSS as our Chief People Officer. In this role, she played a pivotal part in defining and executing an effective talent strategy, strengthening our employer brand, and designing forward-thinking HR policies. Over the last 5 years, Preeti has driven HR Transformation at PLUSS through the strategic use of technology, leading to enhanced performance management, an effective compensation framework, and a culture of learning and leadership development.
Now, Preeti has taken on an exciting new challenge as she transitions to Business Development, focusing on expanding PLUSS’s presence in the Middle East. Her wealth of experience, combined with her passion for building a performance-driven and inclusive culture, makes her the perfect fit for this role.
Outside of her professional life, Preeti is a loving mother and a dedicated philanthropist who believes in the holistic connection of mind, body, and soul. Her journey is a testament to her commitment to excellence in every aspect of life.
Vishnu is passionate, innovative and solution focused professional with a blend of creativity, technical and business experience of 13 years. As the Vice President -New Product Initiatives, he leads the New Business and product development strategies for the Phase Change Material(PCM) business unit with cross-functional responsibilities.
Over the last 8 years in PLUSS, he has been responsible for developing business verticals under PCM from conceptualization stage to scaling up into market. Prior to working with PLUSS he has worked with organizations offering thermal energy storage (TES) solutions in HVAC systems for commercial and industrial buildings, wherein he gained experience of design, engineering, implementation and sales strategies for TES systems.
He holds a Bachelor's degree in Mechanical engineering from Visvesvaraya Technological University, Bengaluru(2007) and MBA in marketing management from S P Jain School of Global Managernent. Singapore and Dubai(2012).
He firmly believes that with focus, discipline and persistence the most complex problem can be solved. He likes to build and implement processes to improve efficiency and is always game to troubleshoot problems irrespective of the department or function. He also believes looking at a problem as an 'outsider and asking the right questions to the customer is the key to solving most problems or arriving at impactful solutions.
His personal interests are in movies, travel, and new technologies. A fitness freak, he starts and ends his day with a customary visit to the gym and has completed two full marathons. He makes sure not to miss any opportunity of participating in a few marathons every year.
Praveen is a dynamic and accomplished professional with over 12 years of experience in the field of Product development, Sales, and Category Management. He has a proven track record of successfully leading teams and delivering exceptional results for his clients and has donned various hats from Service, Product Management, Strategy and Sales through his career. Mr. Das has worked with a wide range of products and is known for his charming networking skills, strategic thinking, and his ability to drive innovation. With a deep understanding of his customers and market trends, Mr. Das has effectively helped drive growth by understanding the pulse of markets very effectively.
Praveen has done his bachelor's in engineering from the Mumbai University and his MBA from the Indian School of Business. He has over a decade of experience in the building materials industry and has worked with Companies like Hafele before joining Pluss. He is excited about the Energy Management sector and is looking forward to developing this space which is the need of the hour.
Praveen is an avid sports enthusiast and was a State level Athlete and Badminton player. In his spare time loves meeting new people, playing badminton, solving puzzles and spending time with his loved ones.
Nidhi graduated in Chemical Sciences and did her post-graduation in Organic Chemistry from St. Stephens College, Delhi University (2005) where she was awarded the best student of the year. In 2007, she submitted her thesis for M.Phil. which focused on 'enzymatic studies of nucleosides' and received the prestigious 'Science Meritorious' award.
Her first job was at the Institute of Genomics and Integrative Biology, Delhi, on chemical synthesis of UV active compounds for DNA labeling. With an eagerness to see her work converted into products, she moved from a pure research environment to an industrial environment at Leonid Chemicals, Bengaluru, where she developed methods for characterization of newly designed chemical compounds. However, in her quest for innovation, she connected with PLUSS. With a belief that energy will be the key to the future, the idea of working on PCMs to store energy appealed to her. What followed was a steep learning curve and over a span of 5 years she built a team and has created several PCMs. Form stable PCM is one of the products which brought a significant change in the pattern of products developed at PLUSS.
Besides, her passion for PCM, she loves plants and her motto is "Be Calm and Go Green". She likes travelling; be it a family outing or an official meeting, she enjoys exploring places and vegetarian food of different origin. Her chemistry experimentation has spilled over to experimenting with cooking too; whether it's a mouth watering dessert or anexotic main course. An avid fiction reader -her favorite authors include Jeffrey Archer, Robin Cook, Harper Lee and Amitav Ghosh.
Apoorv received his integrated master's degree in Polymer Science & Technology from Indian Institute of Technology, Roorkee and a Ph.D. in Chemical Engineering with a focus on energy storage and transport behaviour of glassy ionomers from Clemson University, USA. At PLUSS, he is working on developing new products, materials, applications, and R&D initiatives in the field of energy storage as well as identifying the cost-benefit analysis and value proposition for development of new research and technology verticals.
He is passionate about development of innovative materials which can provide tangible benefits to people and believes in the power of first principles thinking and fundamental data analysis in overcoming any technological challenge. Above all, he considers learning to be his first and foremost responsibility at PLUSS, whereas the ability to do and to achieve are mere by-products.
Apoorv is a philomath and enjoys a wide variety of activities in his personal time. Currently. he is involved in learning to play Kalimba and setting up Raspberry Pi microcomputers for home automation, reading graphic novels and gaming in his free time, and is always happy to discuss current affairs, screenplay techniques and philosophies with anyone interested.
Jan is a people-oriented, passionate pioneer with a broad business and technological background.
He holds a MSc degree in Chemistry (University at Utrecht) and Chemical Technology (Technical University, Eindhoven) and also completed a post academic study of Business Management at Institute for Career & Development in Eindhoven.
Half of his career Jan worked in Pharma and Fine Chemical Industry, in varied roles, as Research Chemist, Head Laboratory, Manager Technology and Business Development Manager. From 2001, Jan worked as Operational Manager/Director in several SME companies in different branches (Agricultural, Chemical, Life Sciences, IT, and Renewable Energy). In these roles Jan was mostly responsible for expanding the business, business development and sales.
Since the beginning of 2019, together with Thijs Veerman, Jan was involved in the development of Pluss Advanced Technologies B.V. where he became Director in January 2020. Jan has agreat interest in technical developments that have positive impact on environmental issues and nature conservation. He is a walking encyclopedia if you want to know anything about gardening and garden plants and trees. He is a member of the Dutch Association of Tub plants and member of the International Clematis Society. In his free time, he does long-distance marches, most 25 miles and once a year even 50 miles.
Gabor holds a B.A. degree in economics from College of Economics and Commerce, Szolnok and has a rich experience in overseas multimodal shipping, warehouse process optimization and retail-chain management. He's also a passionate cook, a music-production enthusiast and a sceptic until proven true. He believes that to help our beloved Earth, it's our responsibility as individuals to 'Reduce and Reuse' as much as we can. His pursuit is to help the industry save on energy and resources by applying advanced methods and technologies.
Eddy holds a B.A. degree in Sales and Management and has a broad experience in concept selling and onboarding projects with several bioproduction companies.
Eddy has knowledge of leading sales teams to meet their goals and targets, working together to mutual goals is what I like best.
In his spare time, Eddy likes gardening, playing badminton and singing in several choirs.
Joris has a bachelor's degree of Business Administration in Hotel Management from the International Hotel School in the Hague. From there he has been active in international business with sports retail, smart urban mobility and tourism. With a focus on Europe as a start, he has been actively pioneering and setting up long-term business relationships in Africa, the Middle East and South America. Now at Pluss Advanced Technologies, he wants to spread sustainable solutions to make the world a greener place. For this, he will be looking for new partners and intensify relations with current business partners who share the same goal. When not behind his laptop, on the phone or traveling the globe for work, you can find Joris in the garden growing his own veggies, on the water windsurfing or in the woods mountain biking. By the way, should you host a dance classics party, you can always invite him to spin some records.
Sonal is a Civil Engineer from Bharati Vidyapeeth University, Pune, and a Postgraduate in Advanced Construction Management from NICMAR, Pune. She is a certified Empowered Entrepreneurship trainer from Johns Hopkins University (SEE Change Initiative).
Sonal has managed building construction, renewable energy, and interior fit-outs projects. In the renewable energy space, her focus was on providing energy access to the rural population and facilitating social impact. She has worked in different domains across strategy, business development, operations, mentoring & training, and project management.
She brings with her a cross sectoral experience held together by one underlying factor which is 'sustainable development'. In addition to her role at Pluss she is a mother of two beautiful girls and a practicing consultant in the area of Energy Access. She loves to paint, and she makes some mouth-watering Indian food.
Samit holds an M.Sc. (Hons.) in Physics and a B.E. (Hons.) in Electrical and Electronics Engineering, both from the prestigious Birla Institute of Technology & Science, Pilani (1994). He also holds a Master of Science degree in Electrical Engineering from the University of Hawai'i, USA (1997).
Samit started his career with Tata Elxsi in India and subsequently worked both at Hawai'i and Los Angeles in the area of network communications before returning to India in 2000. He has been actively involved in various capacities and stages in all functions at PLUSS since 2003. Currently as Managing Director, Samit heads the overall strategy, marketing and finance portfolios. He has led conceptualization and development of various new projects at PLUSS and spearheaded the equity investment of Tata Capital Innovation Fund into PLUSS for development of the current products at PLUSS. He has spoken at several national and international conferences over the years on promoting energy storage and phase change materials.
Extremely passionate about environment, he engages in environment conservation projects with school children as part of Advit Foundation, a not-for-profit organization based in Gurugram. As a trustee of Advit, he has worked extensively to propagate Energy Efficiency and Renewable Energy through various seminars held by GIZ, Germany, Bureau of Energy Efficiency and State Nodal Agencies for Renewable Energy.
Samit would ideally like to create a company based on ethics and values with a culture that will transcend the organization. A company will be known by its people, so people come first for him. Keenly interested in classical music, he hopes to soon find time to start playing the Sitar again. An avid marathoner, with a conviction that good health is the key to success, Samit has successfully completed the Los Angeles Marathon, the Airtel Delhi Half marathon several times and the Standard Chartered Mumbai marathon. He aims to participate in all the major marathons around the world one day!
Sridharan is a member of the Institute of Chartered Accountants of India, a graduate member of the Institute of Cost Accountants of India and holds bachelor's degree in Commerce from Madurai University. Sridharan has about 30 years of overall experience in various fields like banking, manufacturing, contracting, service, and distribution businesses. Sridharan is associated with the Murugappa Group since June 2011 as the Chief Financial Officer of CUMI till January 2018 after which he took over as the President and Group CFO of the Murugappa Group. Sridharan is currently on the Boards of PLUSS, Cholamandalam Financial Holdings Limited, Cholamandalam MS General Insurance Company Limited, Cholamandalam MS Risk Services Limited, Parry Agro Industries Limited, and Net Access India Limited. Sridharan has also served on the Board of Timken India Limited.
Manoj is the Co-Founder and Managing Partner of Symbioteco (www.symbioteco.com), a Singapore based social enterprise, committed to the deployment of sustainability solutions in Asia. He has over 25 years' experience in corporate and investment banking in Asia Pacific and has worked in India, Hong Kong and Singapore. Prior to Symbioteco he was Singapore CEO of IL&FS Financial Services. He has worked with leading global banks such as The Royal Bank of Scotland and ABN AMRO N.V. where he held senior positions such as Head of Corporate Finance and Equity Capital Markets, Asia and Head of Investment Banking, India.
He began his career with Kotak Mahindra in the investment banking group in 1994. He has extensive experience in leading complex M&A and capital market transactions and has a strong network in the Asian financial ecosystem. Manoj has a bachelor's degree in Chemical Engineering and a master's in physics from BITS, Pilani.
Born a natural leader, Manoj lives in Singapore with his wife and daughter. In his spare time Manoj is a student of Vedanta and enjoys meditation and going on long walks.
Harald works independently as consultant, author, and lecturer. He has over 20 years of experience in R&D, with a focus on heat transfer and heat storage, covering materials to applications. He is author of more than 80 publications. He authored one of the bibles on Phase Change Materials - "Heat and Cold Storage with PCM - An up to date introduction into basics and applications" together with Prof. L.F. Cabeza.
He has contributed to several chapters in "Thermal energy storage for sustainable energy consumption - fundamentals, case studies and design". His latest book is "Technologies of energy conversion, storage, and transport in the energy system - A brief introduction". Dr. Mehling received a Diploma and Ph.D. in Physics from University of Würzburg (Germany) - the oldest University in Germany with over 14 nobel laureates in Physics, Chemistry and Medicine to its credit.
He also has a M.S. degree from SUNY Buffalo (USA). Dr. Mehling worked for 15 years at the ZAE, Bayern at Wurzburg and Garching where he was a group leader and senior scientist mainly on Thermal Analysis nalysis and Phase Change Materials.
Designed for bulk shipping, Celsure® XL pallet-in-pallet shippers offer a much larger payload space inside. The payload space in Celsure® XL pallet-in-pallet shippers is configured to easily accommodate one or more standard Euro and/or US pallet shippers for safe, efficient and cost-effective transportation of temperature-sensitive products. The outer size of these shippers is defined keeping in mind the dimensions of the standard ULD in an aircraft.
Celsure® XL pallet-in-pallet shippers are available in all three standard temperature ranges and offer a payload space of over 1000 L up to 2600 L.
Available as both water-based and Phase Change Material (PCM) based, these shippers provide users the flexibility of choosing a perfect solution optimizing the lane risk and cost, and present a superior alternative to traditional shippers and expensive leasing containers
The incorporation of advanced Phase Change Material (PCM) technology offers precise temperature control and a unique hibernating feature that prevents thermal energy loss or gain when stored at the target temperature. This industry-leading innovation is ideal for long-haul multi-modal shipments that encounter delays and are stored at transit points, offering unparalleled temperature stability and reliability.

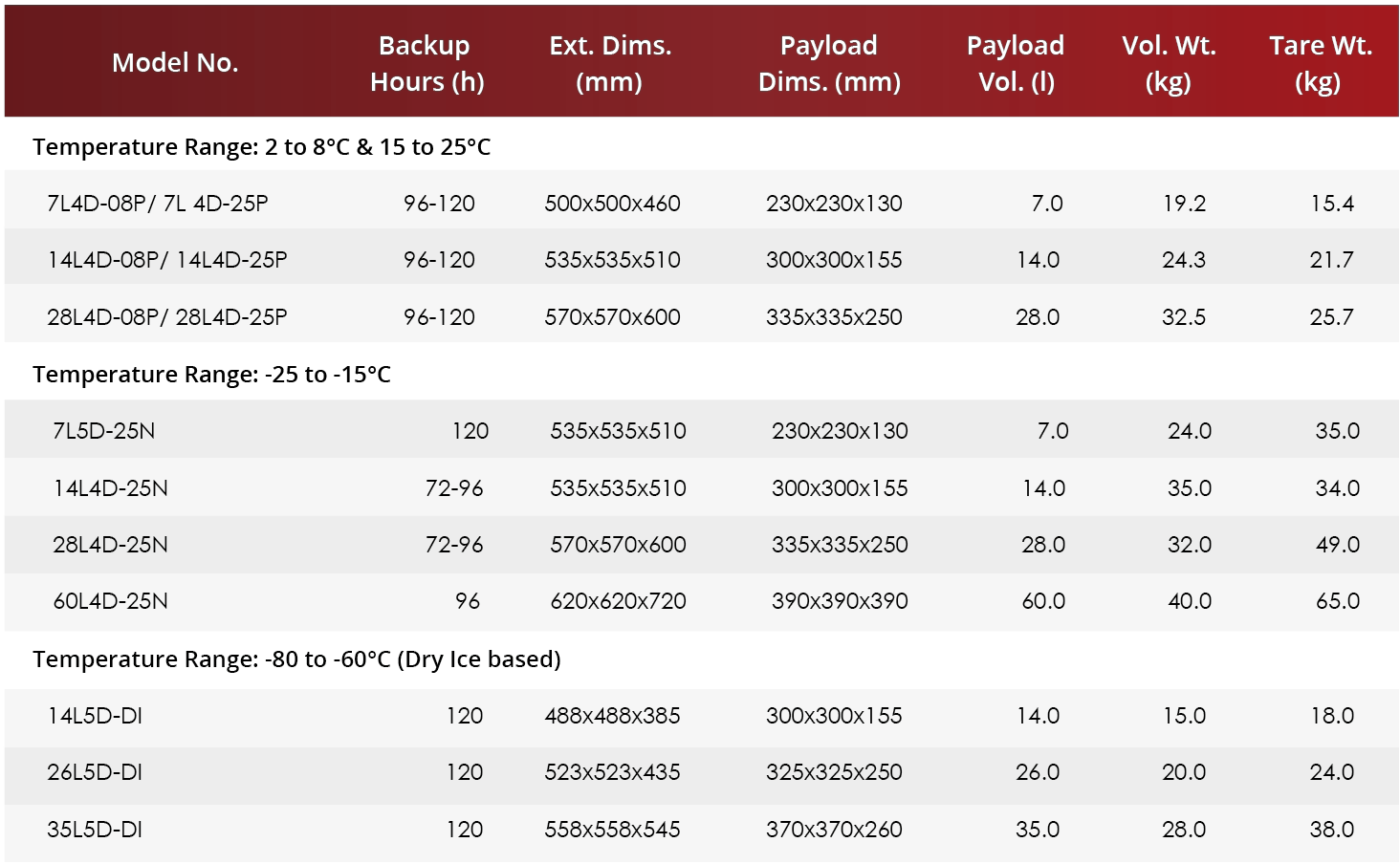
Celsure® and Celsure® Express range of temperature-controlled parcel shippers have been specifically engineered to meet the needs of small to medium domestic and export shipments with payload capacity between 4L to 60L.
The patented and cascaded design of Celsure® and Celsure® Express harness the power of advanced Phase Change Material (PCM) technology. This allows for meticulous temperature control across three key ranges – 2 to 8 degrees Celsius, 15 to 25 degrees Celsius, and -25 to -15 degrees Celsius, ensuring the preservation of product integrity and efficacy throughout the shipment journey.
The standard Celsure® range, with a temperature backup time of up to 120 hours, is designed to meet the demands of export shipments.
On the other hand, the Celsure® Express range, offering a backup of up to 72 hours, is your go-to solution for domestic shipments.



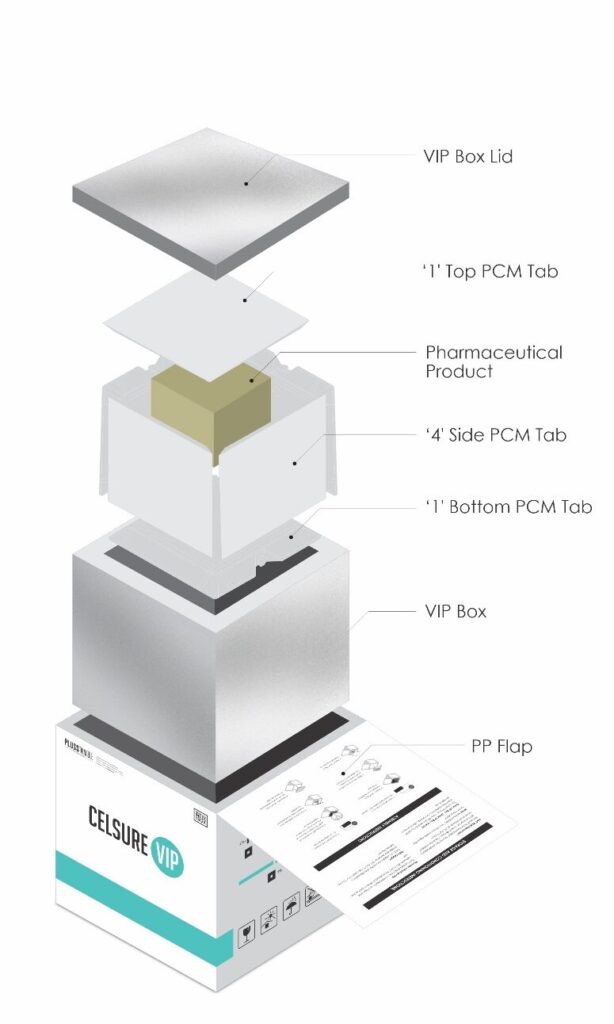
Celsure® VIP shippers are designed for precision for the most sensitive pharmaceuticals, vaccines, and clinical trial samples. These premium shippers embody our commitment to ensure products’ safety and integrity while promoting sustainable and efficient shipping practices.
The powerful combination of Vacuum Insulation Panel (VIP) and Phase Change Material (PCM) technology guarantees that the temperature inside the shippers remains consistent, unaffected by seasonal variations, for extended durations of up to 120 hours. In addition, Celsure® VIP shippers boast a compact design that makes them less than half the size of standard packaging leading to substantial savings on freight costs.
You can also opt for our rental programs for Celsure® VIP solutions to experience the amalgamation of most advanced technology, premium quality, and sustainability.
Most cold chain packaging solutions available in India are made of polystyrene/ polyurethane-based insulation and gel pack-based coolants. Not only are polystyrene and polyurethane-based insulations non-sustainable, they are poorer insulants than vacuum insulation technology. In addition, the traditional use of gel (ice) packs has been poor in precision and longer duration. As a result, India as country has had to live with inefficient and bulky cold chain boxes causing more burden on the cold chain logistics than solving it.
The innovative Celsure VIP replaces the traditional insulant with the VIP insulation which is 10X superior in performance. The VIP insulation housed phase change materials (of different temperatures for chilled, frozen and ambient) to ensure unmatched temperature precision and duration. It does all of this at less than half of the overall size and weight. Pluss has also stayed responsible towards environment by making these solutions as reusable with guarantee of use upto 5 years and offers cooling as a service with this box enabling a circular economy and low cost of technology adoption.
This is India’s first indigenously developed solution with 80% materials sourced locally.


Embrace a sustainable future with Celsure4Earth – an environmentally responsible, efficient, and reliable solution for temperature-controlled pharmaceutical shipping. Combining temperature control with eco-consciousness, Celsure4Earth showcases the seamless amalgamation of functionality and environmental responsibility.
This innovative pharma shipping box, designed to maintain internal temperatures for up to 48 hours, is made entirely of 100% recyclable materials. This leap towards sustainability is a step away from non-recyclable and non-biodegradable EPS (Polystyrene/ thermocol) and PU (polyurethane) insulation-based shippers, which contribute significantly to landfill waste and harm our environment.
For too long, the pharmaceutical industry has been bound by the lack of cost-effective and eco-friendly shipping solutions. Celsure4Earth bridges this gap, providing an environmentally responsible shipping solution without compromising on cost or quality. In addition to using fully recyclable materials, Celsure4Earth boxes are made from materials that are locally available, further reducing carbon emissions associated with long-haul logistics.

